Alternatively, those patients without regular medication were followed-up based on physician decision or after a new event as defined in this study. Patients with regular medication received scheduled follow-up every 1–3 months depending upon their clinical course. Furthermore, the Institutional Review Board at Taipei Veterans General Hospital, Taipei, Taiwan approved this study (VGH-IRB Number: 2013-08- 002AC#1). This methodology has been validated in our previous studies. The final sample included 3767 patients for analysis. The exclusion criteria in our study were as follows: participants with prevalent sustained ventricular tachycardia, permanent pacemaker, heart failure (HF), previous myocardial infarction, catheter ablation, pulmonary hypertension or hypertrophic cardiomyopathy, and valvular heart disease. 
Clinical features for these patients, including past medical history, comorbidities, and medications, were obtained from hospital discharge diagnoses, outpatient visits, emergency visits, and the Collaboration Center of Health Information Application (CCHIA), Ministry of Health and Welfare in Taiwan. The extent of clinical follow-up for each patient was determined by physician decision. A total of 5903 patients were referred for 24-hour electrocardiography (ECG) monitoring between Januand Decemfor the following indications: palpitations, syncope, and suspected arrhythmia hospitalized patients were excluded from the study. This retrospective, observational study was based on the database of “ Registry of 24-hour ECG monitoring at Taip ei Veterans General Hospital” (REMOTE). 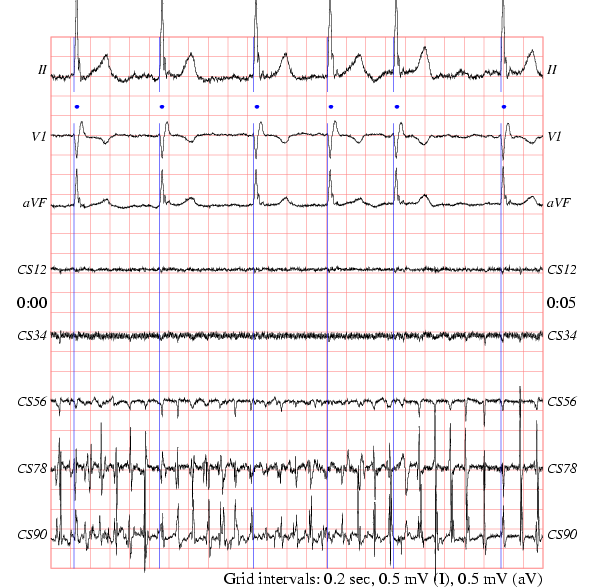
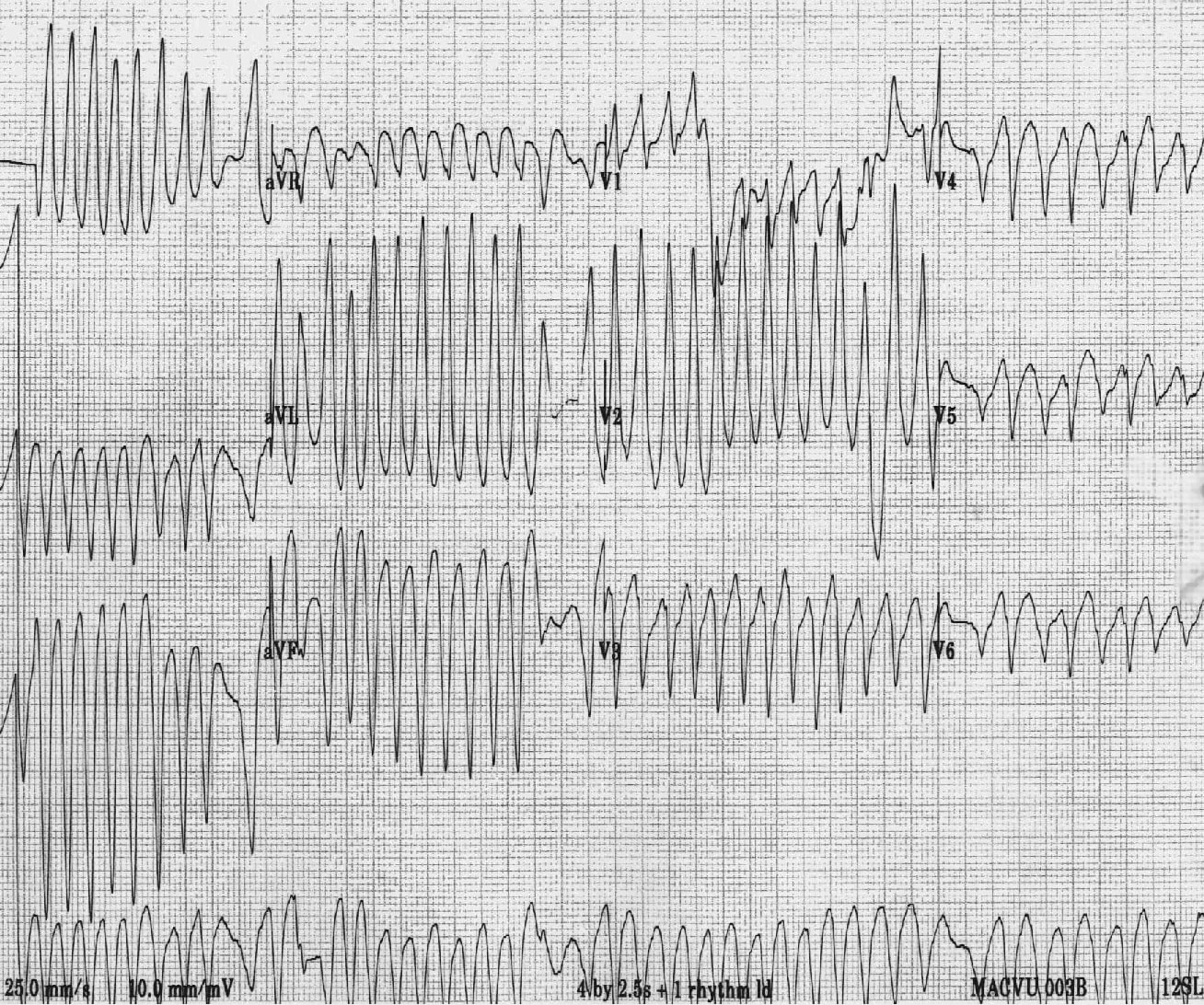
The aim of our study was to evaluate the clinical importance of NSVT in the absence of apparent structural heart disease. These studies suggest that dyssynchronous ventricular contraction might play a role in thromboembolic events. Previous studies showed the association between ventricular arrhythmia and ischemic stroke. The role of NSVT in ischemic stroke is less well-studied, but remains a topic of interest to researchers. Yet the prognostic significance in trained athletes was also controversial in previous studies. During exercise or at the recovery phase, recent clinical studies have shown that NSVT could predict an increase in cardiovascular mortality. However, the prognostic significance of NSVT in structurally normal hearts has not yet been established. Previous studies have suggested an association between NSVT and increased mortality. It has been ascertained that NSVT episodes can be recorded in a normal population. In general, NSVT is defined as 3 or more consecutive ventricular beats with an RR interval of 600 ms and lasting <30 second. If quinidine is administered, it must be preceded by adequate digitalization to produce a sufficient degree of AV block.Non-sustained ventricular tachycardia (NSVT) is a common arrhythmia encountered in modern clinical cardiology. Quinidine, procainamide, or disopyramide must not be used alone for the conversion of atrial flutter to sinus rhythm because these drugs, especially quinidine, increase conduction in the AV node and may result in a 1:1 conduction with a ventricular response exceeding 220/min. Digoxin, verapamil, and beta-blockers are contraindicated in patients with WPW syndrome presenting with atrial flutter. Verapamil or diltiazem is effective in slowing the ventricular response and may occasionally cause conversion to sinus rhythm. Removal of underlying causes may be followed by spontaneous reversion to sinus rhythm. Digoxin converts atrial flutter to AF, and the ventricular response is nearly always slowed to an acceptable level provided sufficient digoxin is used. If underlying heart disease is present, digoxin has a role in the acute and chronic management. The benefit of propranolol or metoprolol is that patients who can undergo electrical cardioversion may do so easily, whereas following digoxin DC shocks have been reported to be hazardous. If the patient is hemodynamically stable with a ventricular response <200/min, propranolol may be used to slow the ventricular response. 
Electrical cardioversion is often indicated and should be performed if the patient is hemodynamically compromised or if the ventricular response is >200/min or the patient is known or suspected to have WPW syndrome. Treatment: Atrial flutter is easily converted to sinus rhythm by synchronized DC shock at low energies of 25–50 J.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
